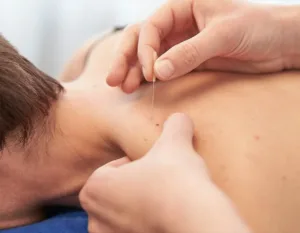
Dry Needling for Pain: Latest Evidence & Safety
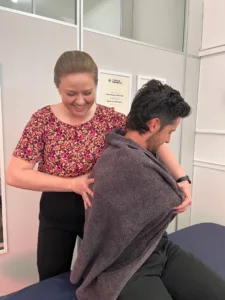
If you’ve ever experienced tight, painful muscles that don’t seem to respond to stretching or massage, you’re not alone. Millions of people suffer from musculoskeletal pain each year, and many are turning to a technique called dry needling as part of their treatment plan. But what exactly is dry needling, and does it really work? Let’s explore what the latest research reveals about this increasingly popular therapy.


 How Pain Disrupts Sleep Quality
How Pain Disrupts Sleep Quality